A case of adult-onset X-linked lymphoproliferative disease mimicking pulmonary infection | BMC Infectious Diseases

A 20-year-old ethnic Han Chinese male was transferred to our center on August 3rd, 2021, for six months of fever with progressive dyspnea and headache. The past medical history was not remarkable. His three elder brothers all died prematurely with fever (at eight-to-twelve-month age), whereas his two elder sisters (aged 33 and 30) were healthy. His parents (aged 62 and 60) were both healthy.
The patient developed unproductive cough and shortness of breath six months before admission (February 2021). The symptoms gradually worsened despite oral antibiotics administered by the community clinic, and he developed fever with chills two weeks later (maximum body temperature 38.5℃). Chest computed tomography (CT) on March 6th revealed bilateral diffused nodules of various sizes, with marked consolidation in the lower right lung (Fig. 1A, upper panel). Mediastinal lymphadenopathy and splenomegaly were also present. The complete blood counts and white blood cell differentials were all within normal range. Metabolic panel revealed elevated transaminase levels (alanine aminotransferase [ALT] 100 IU/L, aspartate aminotransferase [AST] 123 IU/L). The arterial blood gas analysis showed type I respiratory failure. Anti-nuclear antibodies (ANA) and blood cancer biomarkers were all negative. The immunoglobulin levels were within normal range. The C-reactive protein (CRP) was slightly elevated (11.90 mg/L, normal range < 10 mg/L), but serum pro-calcitonin (PCT) was within normal range. Tests for human immunodeficiency virus, hepatitis B virus, and hepatitis C virus were all negative. The interferon-γ release assay for tuberculous was also negative. EBV DNA or antibody was not tested. He was given intravenous broad-spectrum antibiotics and empirical oral anti-tuberculous treatment, but his condition continued to worsen. He was intubated with mechanical ventilation and supported with extracorporeal membrane oxygenation (ECMO). The microbiologic culture tests as well as pathogen next-generation sequencing (NGS) were all negative on peripheral blood, bronchoalveolar lavage fluid (BALF), or cerebrospinal fluid (CSF) samples. Lung biopsy revealed consolidation, damage of alveolar structure, and fibrinous exudate with infiltration of histiocytes and lymphocytes (Fig. 1C). No pathogen was detected by pathological studies, and Epstein-Barr encoding region (EBER) in situ hybridization was negative in lung biopsy sample. Empirical broad-spectrum anti-bacterial, anti-fungal, and anti-viral treatment were initiated with limited clinical improvement (Fig. 2). A tentative glucocorticoid pulse therapy (500 mg/d × 3d) was then administered (Fig. 2) and his conditions gradually stabilized. Chest CT on May 12th showed that pulmonary lesions partially resolved (Fig. 1A, lower panel). The glucocorticoid dose was gradually decreased, and he was discharged in June, 2021, without fever or shortness of breath. He developed fever again one month later (July 2021) with episodes of headache and blurred vision. Brain MRI showed sporadic intracranial lesions with enhancement. Lumbar puncture was negative. His blood test was weakly positive for cryptococcal antigen, but CSF cryptococcal test was negative. Sputum culture was positive for pan-resistant Actinobacter baumannii. He was treated with combination of broad-spectrum antibiotics, fluconazole, and glucocorticoid. His temperature became normal, but his neurologic symptoms persisted with newly-developed numbness in extremities.
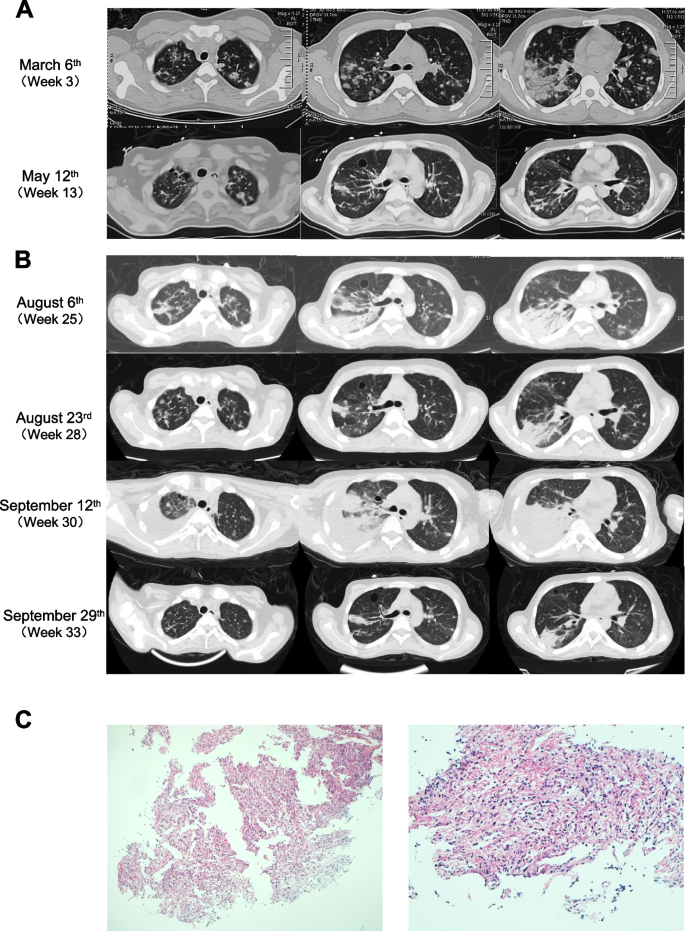
Clinical images of the patient. A Chest computed tomography (CT) of the case before admission. The patient was presented with bilateral nodular lesions in the lung, with consolidation in lower right lung (upper panel). The lesions partially resolved after steroid therapy (lower panel). B Chest CT images of the case in our center. The pulmonary lesions partially resolved after treatment of fluconazole and amphotericin B (8–6 to 8–23). The recurrence of pulmonary lesions was in parallel with rise in body temperature (9–12), and resolved again after strengthened steroid therapy (9–29). C Pathological studies of lung biopsy. H&E means Hematoxylin–Eosin staining. Cluster of differentiation 3 (CD3) is a surface marker for T lymphocytes. KP-1 stains CD68, which is marker of histiocytes. D Brain MRI images of the patient (T2 flair), showing multiple lesions in periventricular and sub-cortex regions
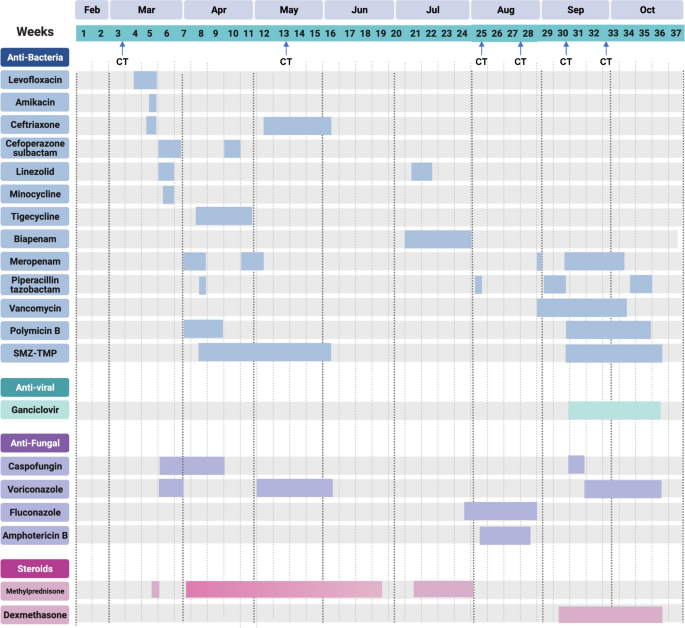
Anti-infective and steroid treatment. The medication information was collected from printed medical records and verified with the patient. All medications were administered based on manufacturer-provided instructions. The glucocorticoid pulse therapy was started as 500 mg methyl-prednisone qd, and gradually reduced to 20 mg qd. SMZ-TMP stands for sulfamethoxazole and trimethoprim
The patient was transferred to our center on August 3rd, 2021 (week 25 from disease onset). Body mass index (BMI) on admission was 15.7 kg/m2. Physical examination revealed reduced respiration in right lower lung and bilateral rales. A contact history with pigeons before disease onset was confirmed. A repeat lumbar puncture was inconclusive. The patient was clinically diagnosed as cryptococcal pneumonia and cryptococcal meningitis, and was given intravenous fluconazole plus amphotericin B despite lack of definite microbiological evidence. His neurologic symptoms gradually resolved, and pulmonary lesions partially resolved on chest CT (Fig. 1B, first two rows). His body temperature was normal and there was no complaint of shortness of breath.
He developed fever again on day 25 after admission with maximum body temperature being 40℃. Blood culture was positive for methicillin-resistant Staphylococcus aureus (MRSA), and sputum culture was positive for carbapenem-resistant Actinobacter baumannii (CRAB), Pseudomonas aeruginosa, and Aspergillus flavus. Blood CMV and EBV DNA were negative, but the serum EBV-IgG was positive. Differential white blood cell count showed markedly reduced neutrophil counts and agranulocytosis was persistent (lowest peripheral blood neutrophil count being 0.01 × 109/L). Hemoglobin (lowest being 63 g/L) and platelet cell counts (lowest being 17 × 109/L) were also below normal range. Chest CT showed relapsed pulmonary lesions and new pleural effusion in right lung (Fig. 1B, third row). Broad-spectrum anti-bacterial and anti-fungal treatment including polymyxin B was soon initiated (Fig. 2). Ganciclovir was given as preventive anti-viral treatment in immunocompromised host. Bone marrow biopsy revealed hemophagocytes and elevated recruitment of T lymphocytes. Serum ferritin (1199.1 ng/ml, normal range < 336.2 ng/ml) and sCD25 (17539 pg/ml, normal range < 6400 pg/ml) was greatly elevated. The NK cell activity was normal (28.71%, reference range > 15.11%). Serum fibrinogen was slightly elevated (4.05 g/L, normal range 2–4 g/L). Hemophagocytic lymphohistiocytosis (HLH) was diagnosed. A combination of intravenous dexamethasone (10 mg/m2/d) and etoposide (45 mg/m2 per week) were administered based on the HLH-1994 regimen (Fig. 2), except that the dose of etoposide was reduced due to pre-existing myelosuppression. Blood transfusion was initiated as supportive to aplasia anemia (in total 8U red blood cell, 18U platelet, and 2000 ml fresh frozen plasma). His body temperature returned to normal and neutrophil count gradually increased to 1.07 × 109/L after two weeks of HLH and anti-infective treatment. The pulmonary nodules and consolidation also partially resolved (Fig. 1B, last row). However, his conditions quickly relapsed after dexamethasone dose was reduced to 5 mg/m2/d. His serum ferritin continued to rise (> 15000 ng/ml). The serum total glycerol (2.92 mmol/L, normal range < 1.70 mmol/L) was elevated, indicating that HLH was still active. He developed acute liver and kidney failure one month after HLH onset and the anti-infective regimen was withdrawn due to potential drug-induced organ failure. He quickly developed fever after the removal of broad-spectrum antibiotics. Sputum culture was positive for carbapenem-resistant Pseudomonas aeruginosa (CRPA). Blood culture test was refused. The patient was discharged against medical advice on day 80 after admission (week 36 from disease onset). He died of septic shock two days later (2 months after HLH onset).
The patient’s peripheral blood sample was acquired and whole-exon sequencing was performed. He was found to carry a nonsense mutation in SH2D1A gene (c.163C > T, p.Arg55*) in the X chromosome, which has been associated with X-linked lymphoproliferative disease type 1 [8]. Sanger sequencing was performed to confirm the mutation, and both his parents were tested for this mutation by Sanger sequencing. His mother was heterozygous for this mutation, and his father was wild-type. One of his two sisters also carried this mutation. The other family members were not tested. The pedigree chart and sequencing results were shown in Fig. 3. Further pathological investigations on the lung biopsy samples revealed proliferation of non-Langerhans histiocytes (CD1a negative, CD68 positive) and CD3-positive T lymphocytes. Only a few B lymphocytes were observed. There were few S-100 positive cells and scattered Cyclin D1 positive cells. Periodic Acid-Schiff [PAS] staining and silver staining were negative. The Ki67 index was about 20%. The sample was positive in clonal recombination in T cell receptor (TCR)-B, D, and G genes, but not in IgH, IgL, or IgK gene segments.
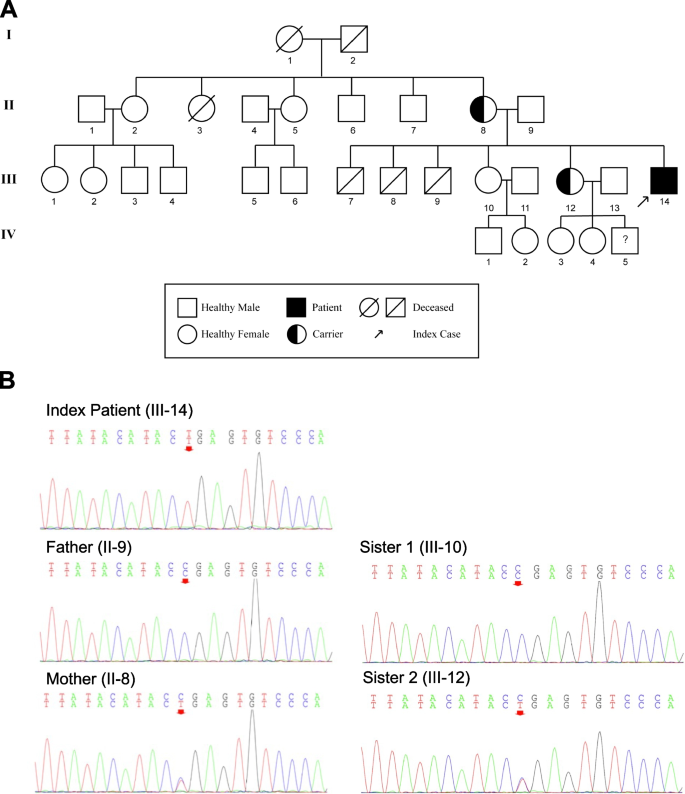
Pedigree and Sanger sequencing verification. A Pedigree information was collected from interviewing with the patient. The index case (III-14) was shown with an arrow. His parents (II-8 and II-9) as well as two elder sisters (III-10 and III-12) were tested for the mutation with Sanger sequencing. The patient’s mother (II-8) and one of his sisters (III-12) were carriers. Genetic testing of generation IV was refused. By the publication of this manuscript, IV-1 to IV-4 were 15, 8, 8, and 7 years old and were all healthy. The question mark in IV-5 indicated an uncertain status of disease because genetic testing was refused (2-year old infant)
link